IDHEAL
Social Emergency Medicine Teaching Modules
This work is licensed under the Creative Commons Attribution-No Derivatives 4.0 International License
BUILT ENVIRONMENT
Module 15
Vanessa Kreger, MD, MPH
Objectives
1. To consider the ways in which the built environment and urban design affect health outcomes and health care utilization.
2. To foster discussions of the role that emergency medicine providers play in addressing health disparities associated with the built environment.
3. To understand what resources are available to help patients with the built environment.
Case
An 8-year-old boy with a history of asthma and allergic rhinitis is brought into the emergency department by his mother for persistent wheezing and increased work of breathing over the last hour despite strict medication compliance. This is the patient’s third presentation to the ED over the last 8 months with one ICU admission in the last year. In addition to these ED visits and hospitalizations, the patient’s mother expresses concern about her son’s worsening school attendance due to frequent asthma exacerbations. The patient is up to date on all childhood vaccinations and lives in a non-smoking household. The patient and his family live about a quarter of a mile away from a major freeway interchange in a densely populated urban community. The patient’s school is near dense urban traffic corridors as well. Both of the patient’s siblings also have poorly controlled asthma despite optimal medical management and health education.
While in the ED, the patient’s symptoms were appropriately medically managed with improved work of breathing and decreased wheezing throughout bilateral lung fields. Upon discharge, the patient’s mother desperately inquired what more she could do to help prevent further such exacerbations in the future. The patient’s physician acknowledged the mother’s consistent work to control the patient’s asthma. The provider described environmental and structural causes and triggers to asthma, including proximity to dense urban traffic corridors. The physician encouraged on-going strict medication compliance and offered new ideas to better control the patient’s asthma, including avoiding outdoor-play during peak traffic hours. The practitioner explored the eventual possibility of the family relocating further to a neighborhood with less dense air pollutants and traffic. It is important for the provider to recognize frequent barriers to relocation including socioeconomic status, employment, family, transportation, etc.
Discussion Questions
1. What is the built environment?
2. How does the built environment affect health?
3. What can ED do to address challenges with the built environment?
Teaching Points
1. The built environment is described as the man-made, physical attributes of our surroundings, including structural conditions affecting walkability and recreation, availability of health-promoting resources (e.g. grocery stores, parks), undesirable amenities (e.g. fast-food restaurants, liquor stores, marijuana dispensaries) that influence individual and community health behaviors (physical, activity, diet).
2. A growing body of evidence points to the important role that poor built environment (ex. dense urban traffic corridors, food deserts, ‘un-walkable’ neighborhoods, poor, overcrowded, old housing structures, etc.) plays on a multitude of health outcomes including asthma, obesity, cardiovascular health, maternal and fetal health, and neurologic health. It is important to understand and acknowledge structural and systemic barriers to health that disproportionately burden certain neighborhoods, most frequently low-income communities.
3. The built environment has a direct impact not only on health outcomes but health care utilization as well. For example, studies indicate that individuals who reside in dense urban traffic corridors with high concentrations of air pollutants and small particulate matter have higher prevalence of poorly controlled asthma. As such, these individuals present to EDs and utilize healthcare at higher rates than their counterparts who lack this exposure.
4. On an individual level, ED physicians can acknowledge the challenges their patients face and offer creative solutions to mitigate the effects of the built environment. On a larger scale, it will require a multi-disciplinary approach involving health care providers, city planners, economists, health policy experts, environmental scientists, community advocates, etc. to advocate for policies that support healthy built environments and environmental justice.
Practical Questions
(The responses may be modified to your own hospital/clinical environment. Example responses below refer to the UCLA-Olive View Medical Center Emergency Department.)
1. Think about communities surrounding your emergency department. Discuss the role of the built environment on community health (consider childhood asthma, for example). What other features of the built environment impact patient health?
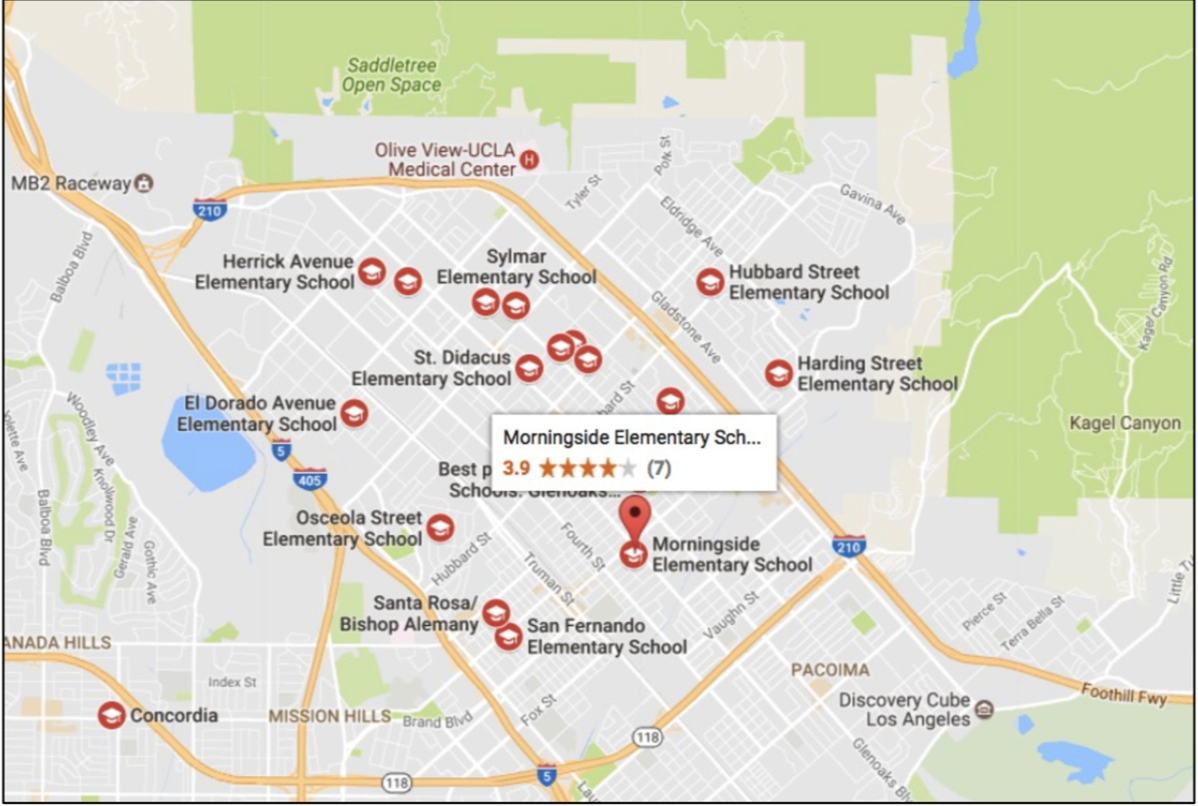
Olive View-UCLA Medical Center is located within the densely-populated LA Basin, a region with some of the worst traffic congestion and air pollution in the world. OVMC is located at the base of the San Gabriel Mountains in a region of the LA Basin where air pollutants tend to accumulate in greater density as compared to other regions of Los Angeles. As such, the communities that make up the area around OVMC bear a substantial health burden of the poor regional air quality. As demonstrated by the map below, elementary schools in this region are surrounded by some the heavily driven highways. This contributes to a disproportionate health burden on young children and their lungs.
3. Are there local groups one can partner with to advocate on behalf of improving the built
environment?
Recommended Screening Question(s)
The LA County Health Agency SBDOH workgroup has not developed any recommended screening questions for this domain.
Paired Reading
Brandt, Sylvia, Laura Perez, Nino Kunzli, Fred Lurmann, John Wilson, Manuel Pastor, Rob McConnell. “Cost of near-roadway and regional air pollution—attributable childhood asthma in Los Angeles County.” Journal of Allergy and Clinical Immunology 134 (2014): 1028-1035.
Discussion Points from the Reading
1. Near roadway air pollution can cause childhood asthma.
2. Costs of near roadway air pollution can be significant including direct costs for
healthcare, and indirect costs such as lost wages.
3. Los Angeles County's rate of childhood asthma is particularly high and attributions have
been made to dense traffic corridors, regional air pollutants such as ozone, nitrogen dioxide and particulate matter.
Additional Readings
1. Delamater, Paul L., Andrew O. Finley, Sudipto Banerjee. “An analysis of asthma hospitalizations, air pollution, and weather conditions in Los Angeles County, California.” Science of the Total Environment 425 (2012): 110-118.
2. Huynh, Peter, Muhammad T. Salam, Tricia Morphew, Kenny Y. C. Kwong and Lyne Scott. “Residential proximity to freeways is associated with uncontrolled asthma in inner- city Hispanic children and adolescents.” Journal of Allergy (vol. 2010, Article ID 157249, 7 pages, 2010. doi:10.1155/2010/157249.
3. Koppel, Lianna S., Wanda Phipatanakul, Jonathan M. Gaffin. “Social Disadvantages and Asthma Control in Children.” Paediatric Respiratory Review 15.3 (2014): 256-63.
4. Kranjac, Ashley W., Rachel T. Kimbro, Justin T. Denney, Kristin M. Osiecki, Brady S. Moffett, Keila N. Lopez. “Comprehensive Neighborhood Portraits and Child Asthma Disparities.” Maternal and Child Health Journal (2017): 1-11.
5. Largent, J, B. Nickerson, D. Cooper, R.J. Delfino. “Paediatric asthma hospital utilization varies by demographic factors and area socio-economic status.” Public Health 126 (2012): 928-36.
6. Mazenq, Julie, Jean-Christophe Dubus, Jean Gaudart, Denis Charpin, Antoine Nougairede, Gilles Viudes, Guilhem Noel. “Air pollution and children’s asthma-related emergency hospital visits in southeastern France.” European Journal of Pediatrics (2017). Doi 10.1007/s00431-017-2900-5.
